Papillary eccrine adenoma & tubular apocrine adenoma are very similar and some authors combine the two entities under the umbrella term “tubular adenoma”. While this has merit, there are clinical differences. Papillary eccrine adenoma arises most often on the extremities and shows a marked predilection for black females (9F:1M). Tubular apocrine adenoma most commonly arises on the scalp & very rarely affects the extremities. Tubular apocrine adenoma is characterized by decapitation secretion, papillary eccrine adenoma is not. Tubular apocrine adenoma shows GCDFP-15 expression, papillary eccrine adenoma does not. However, supporting the hypophysis that they are very closely related is the report that both tumors share BRAF & KRAS mutations (Liau et al 2018)

Clinical features
•Rare tumor showing a predilection for the scalp but may arise in the eyelid, on the face, axilla and elsewhere
•Dermal nodule (1-2 cm)
•Genital lesions are best regarded as tumors of the anogenital mammary-like glands
•A relatively common tumor arising in nevus sebaceus
•2F:1M
.Wide age distribution
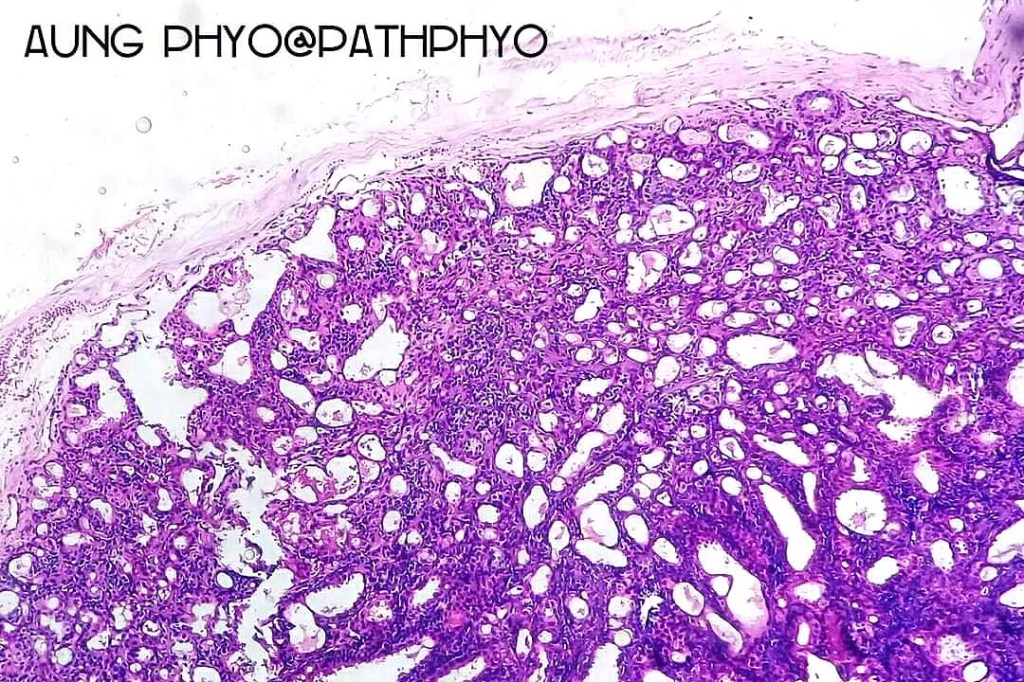
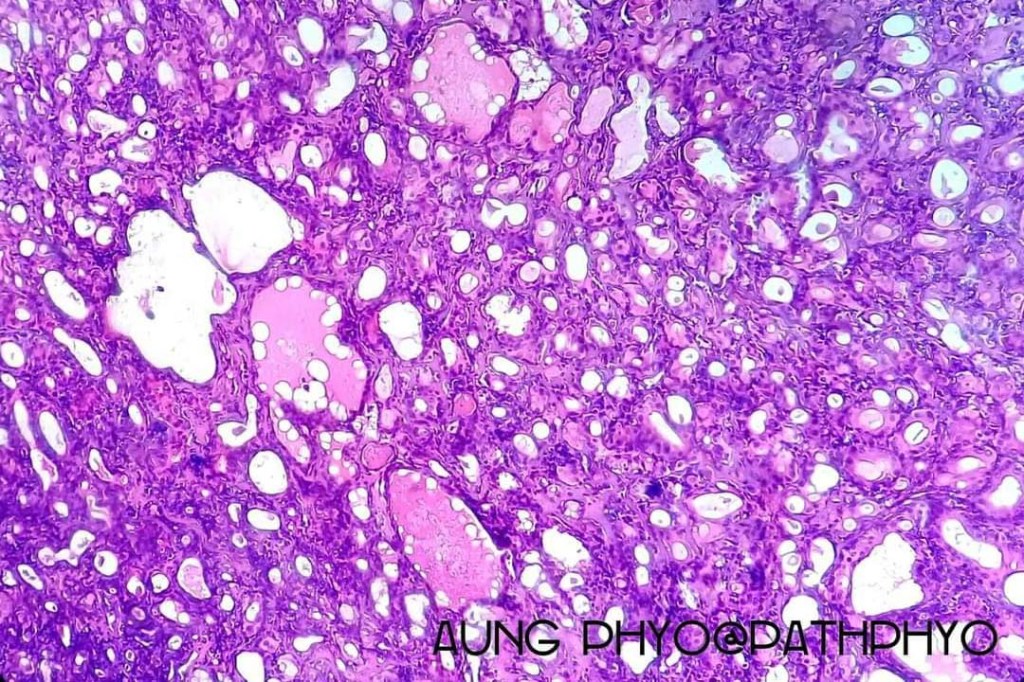
Histological features
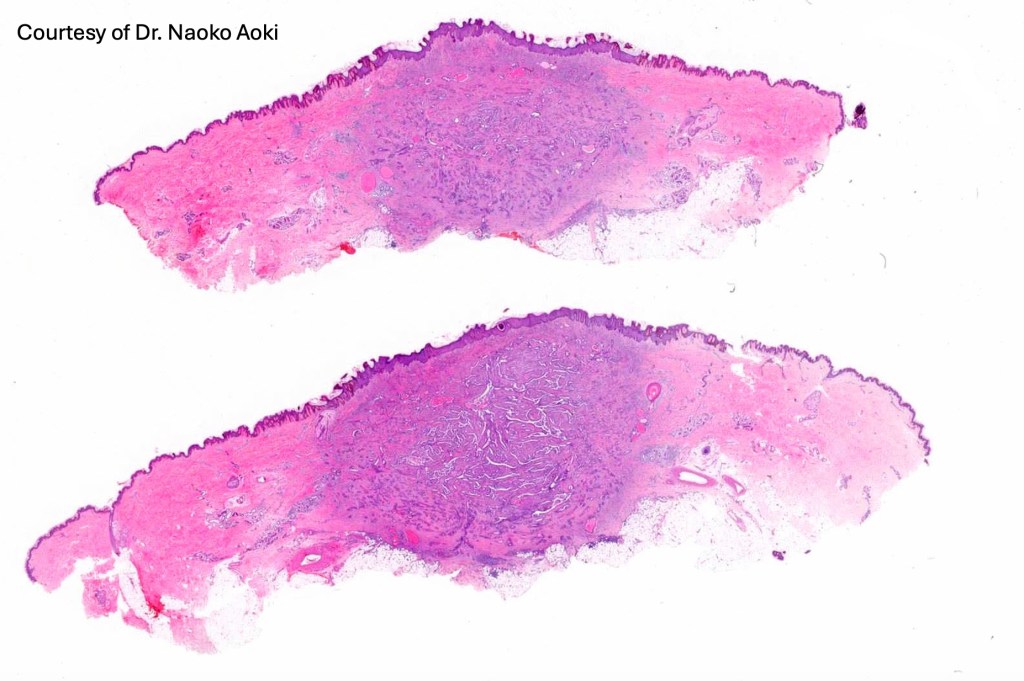
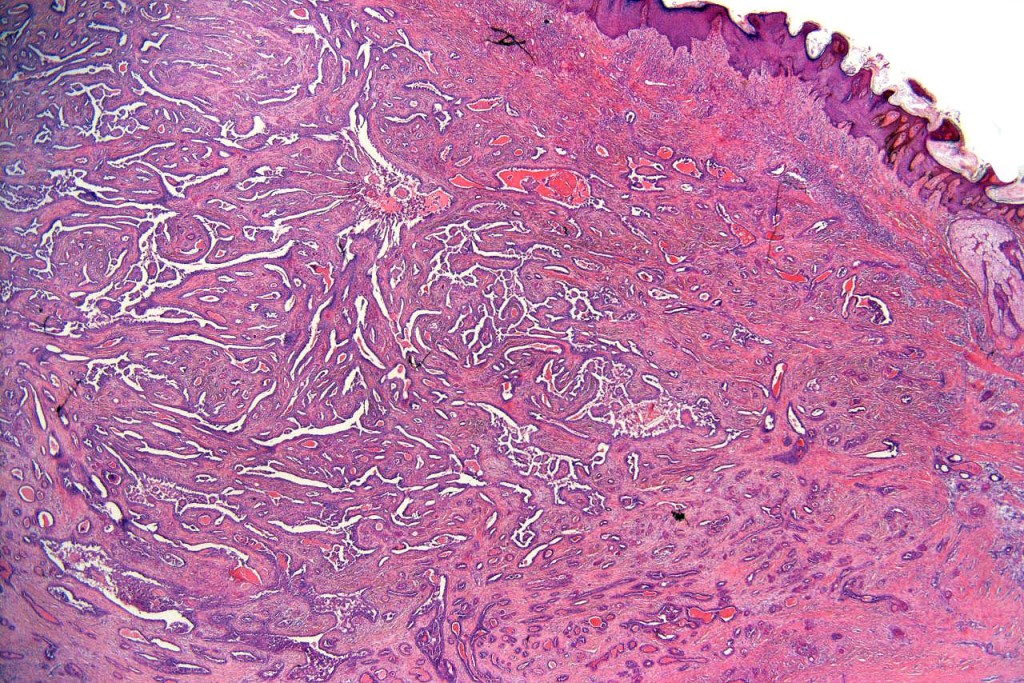
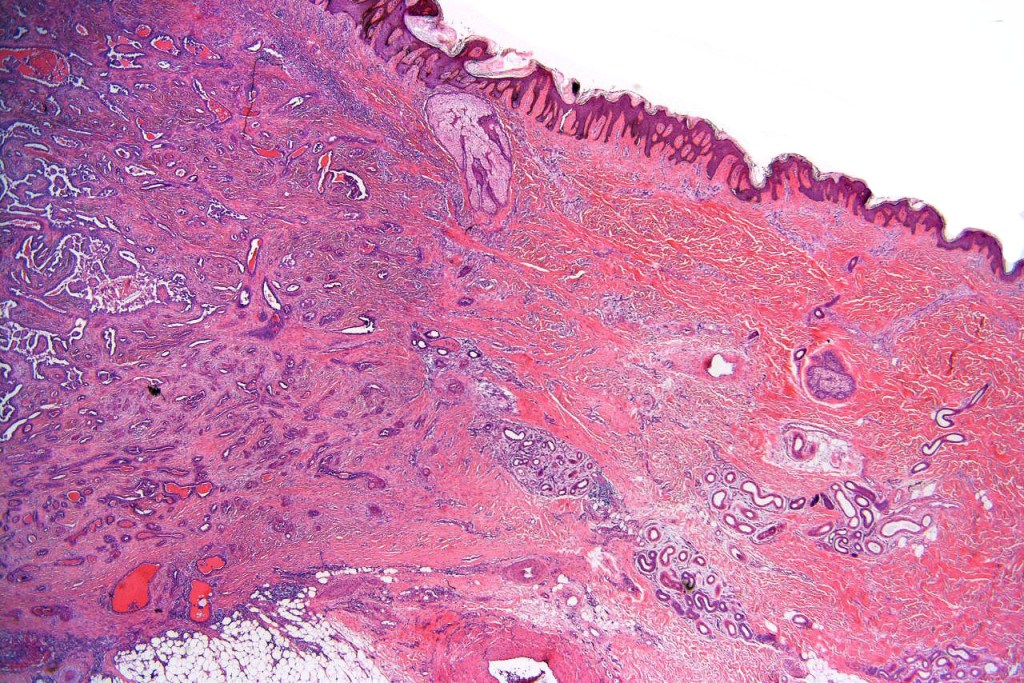
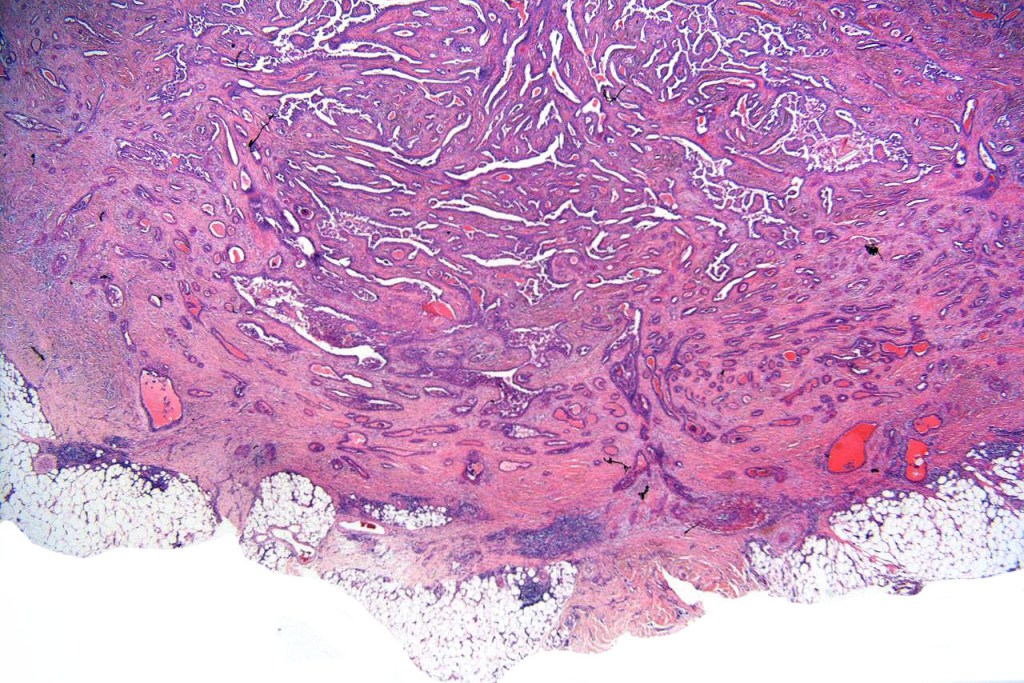
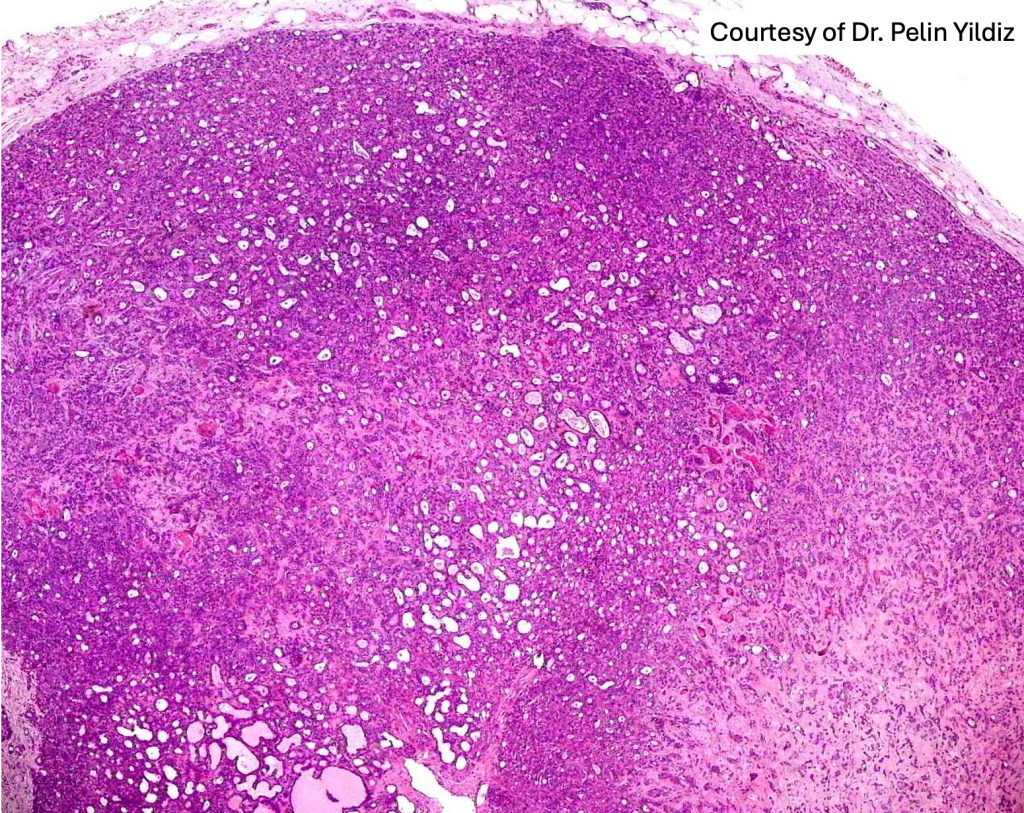
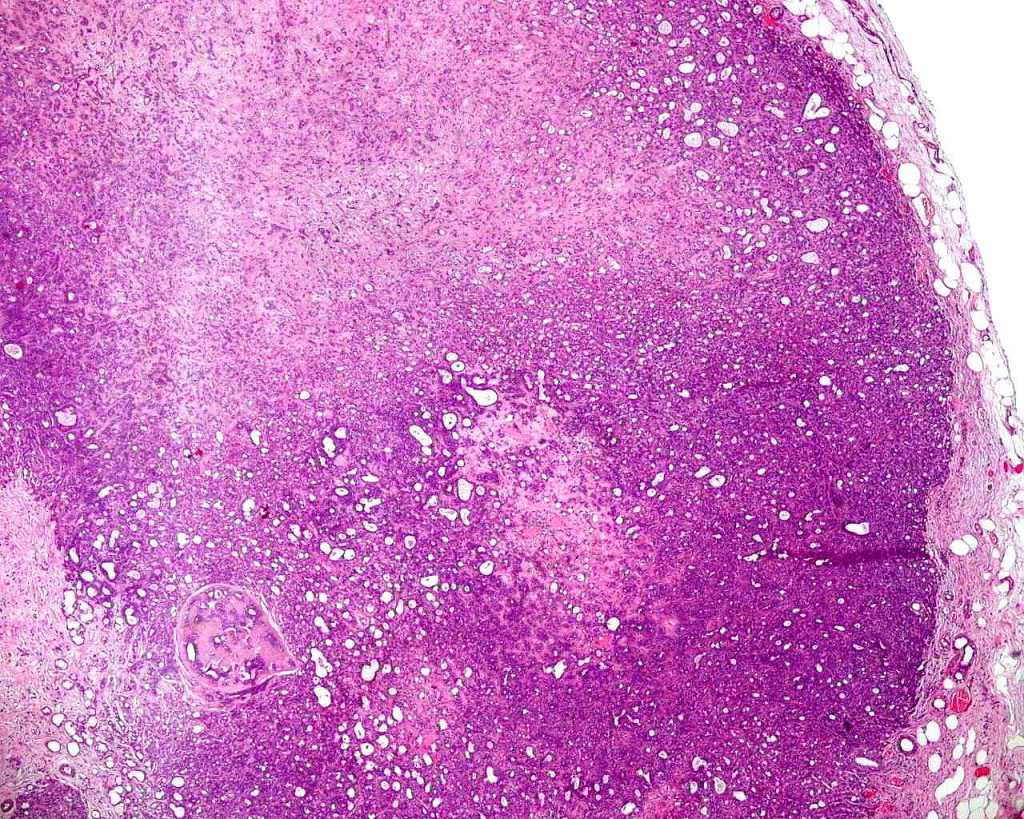
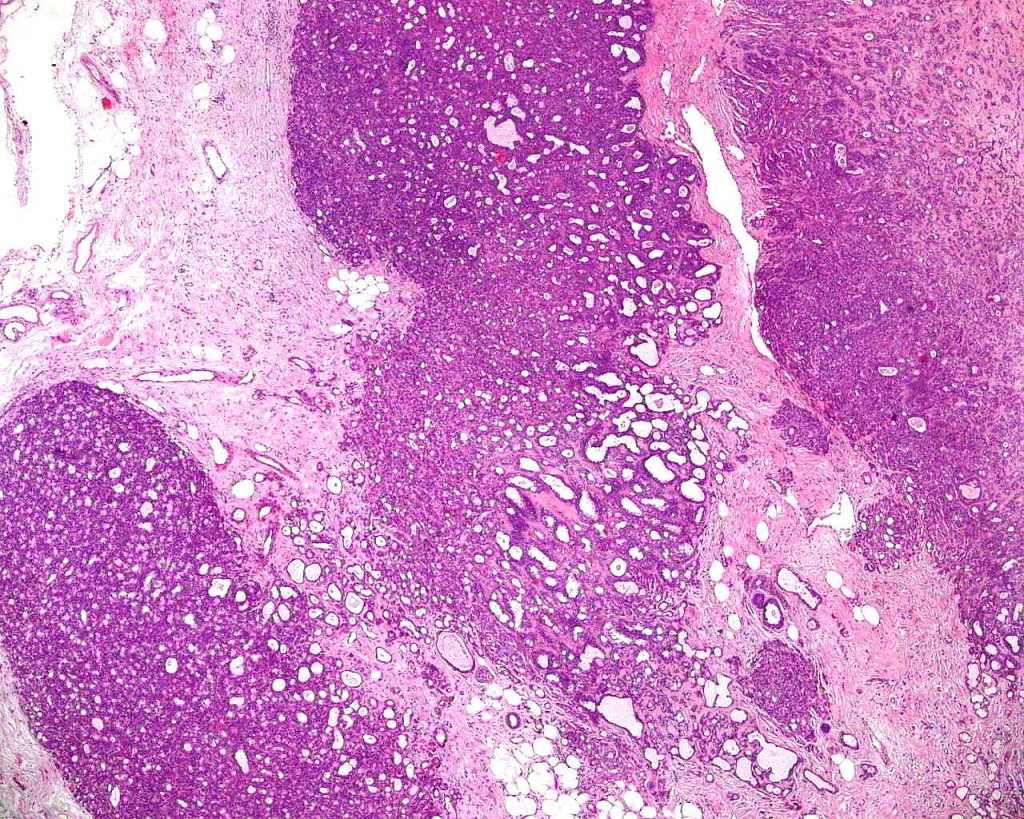
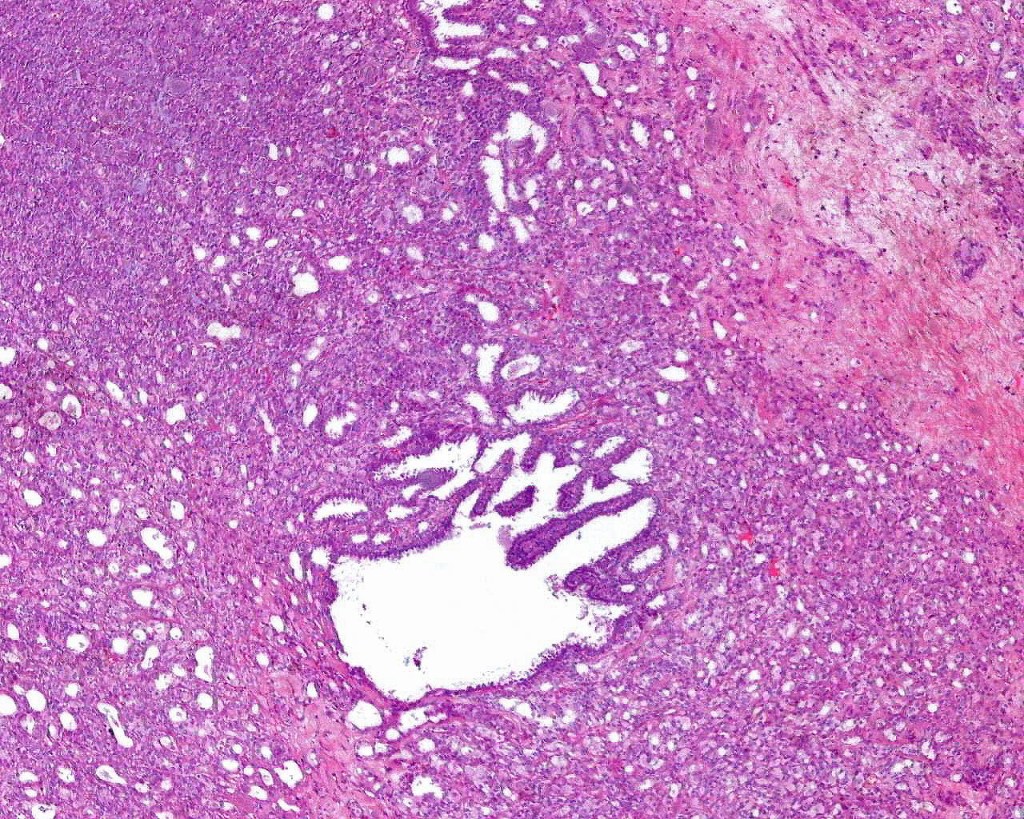
•Dermal nodule
•May communicate with epidermis/follicle- also arise below a syringocystadenoma papilliferum
•Some tumors may overlap syringocystadenoma papilliferum/hidradenoma papilliferum
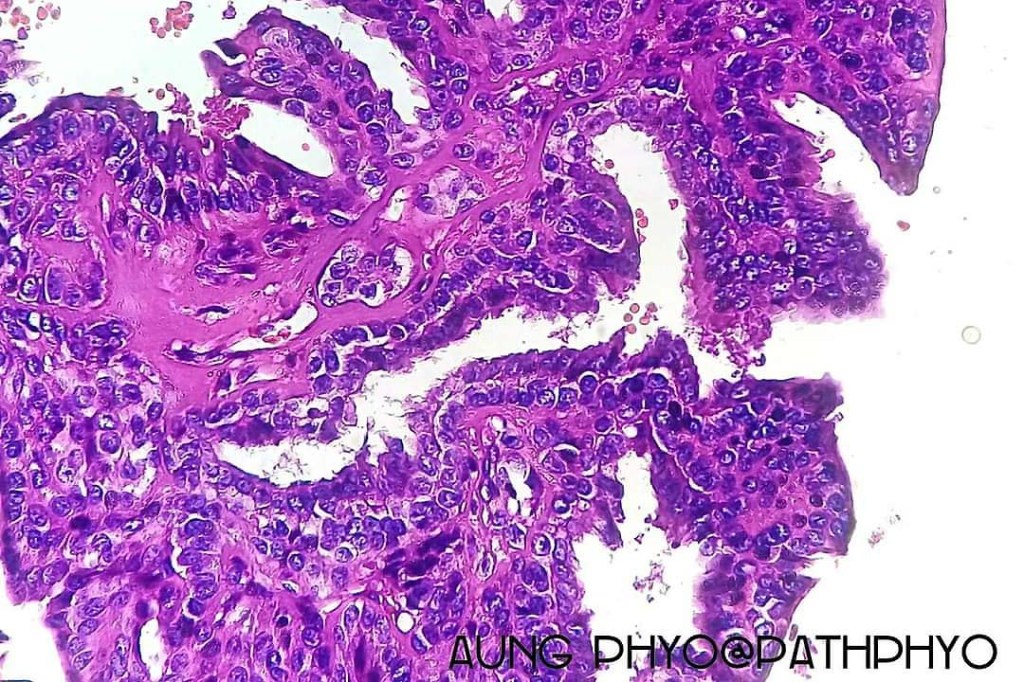
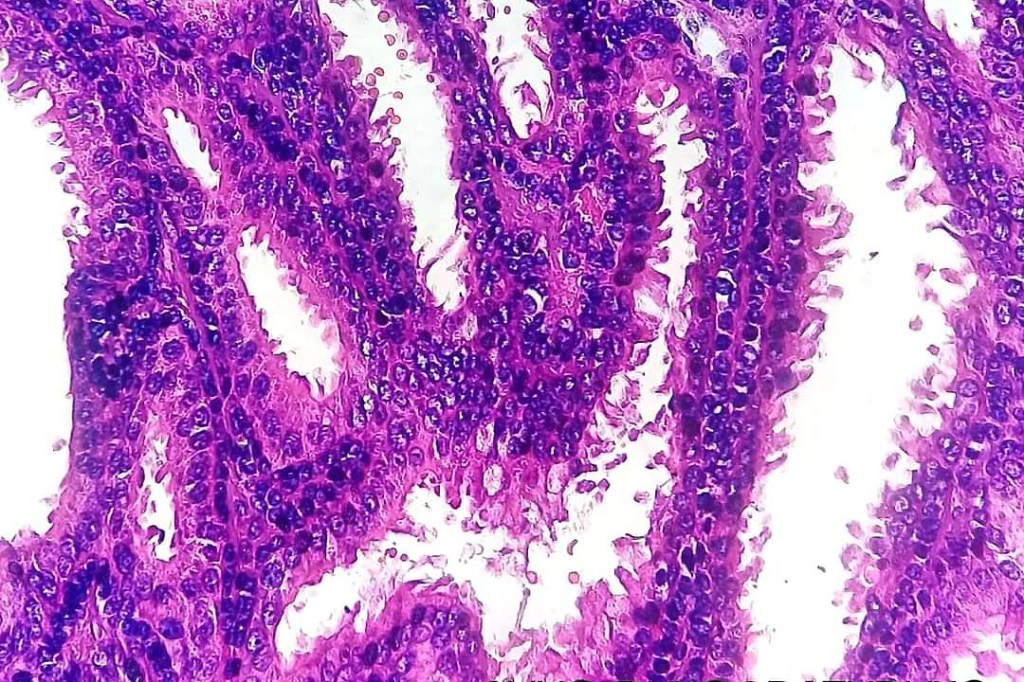
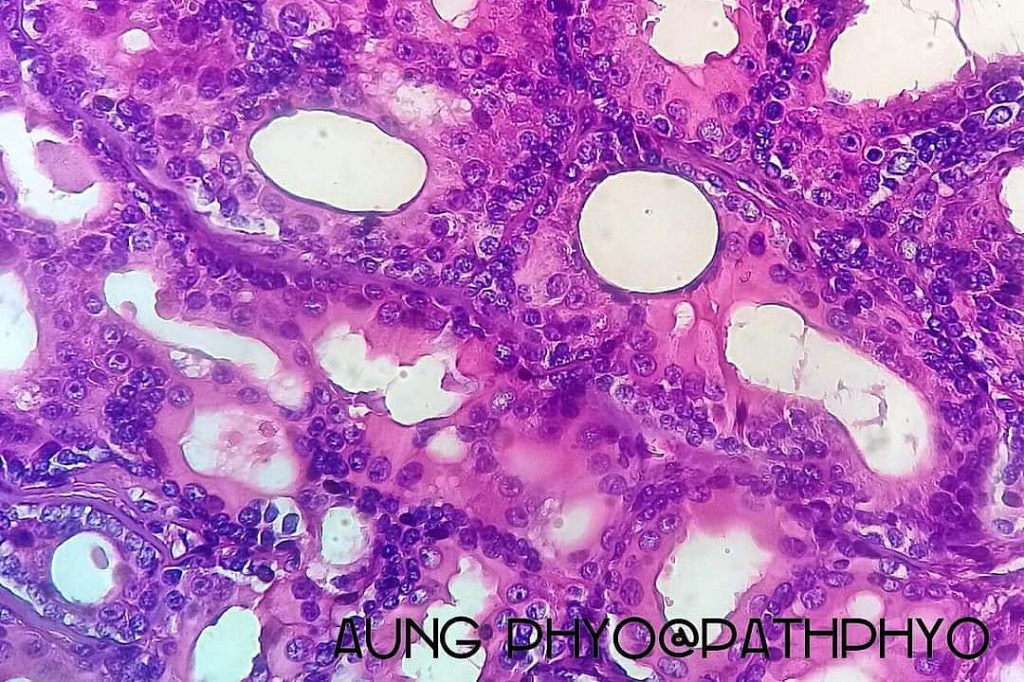
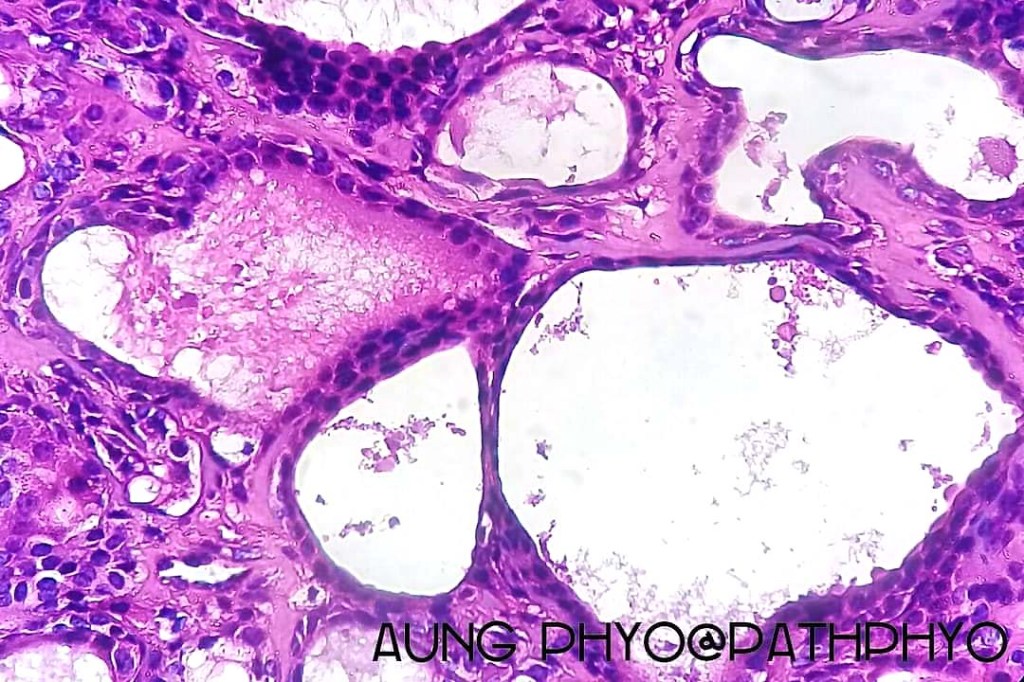
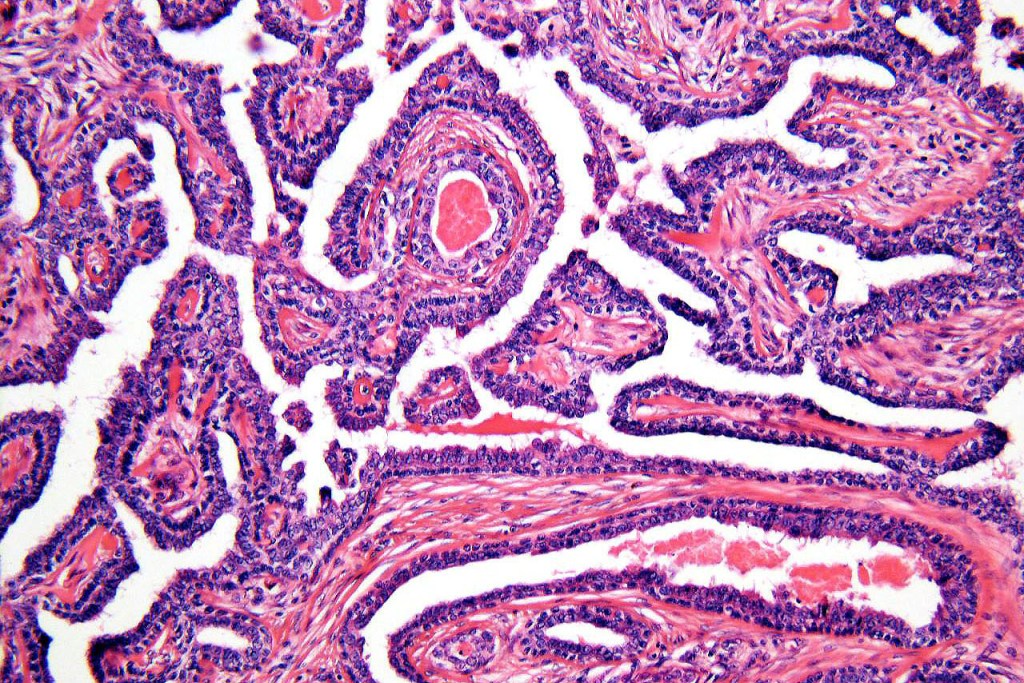
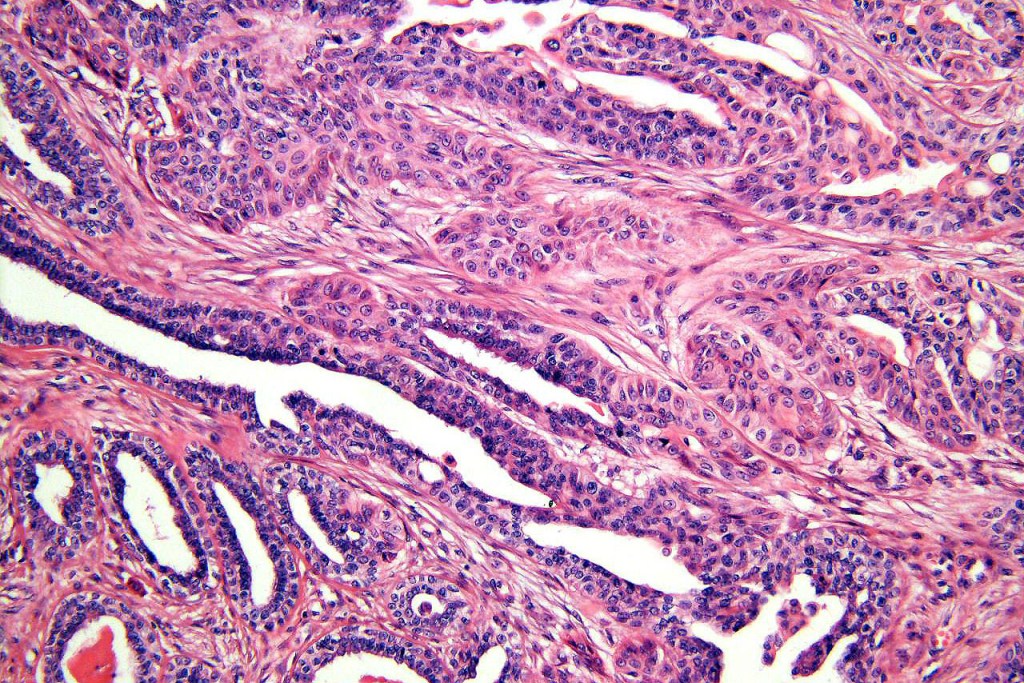
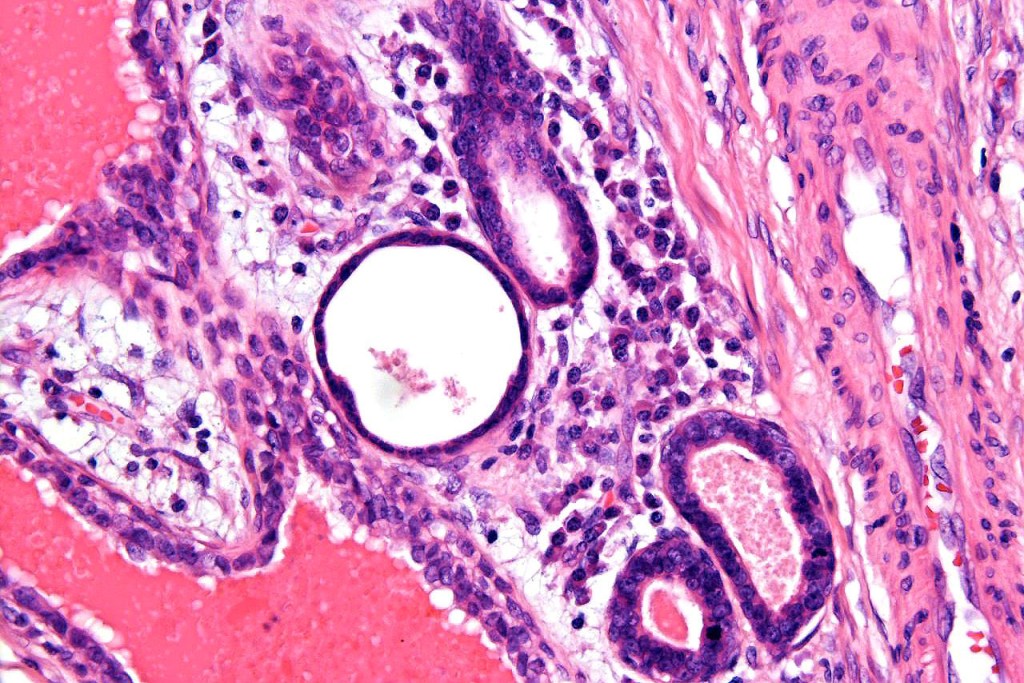
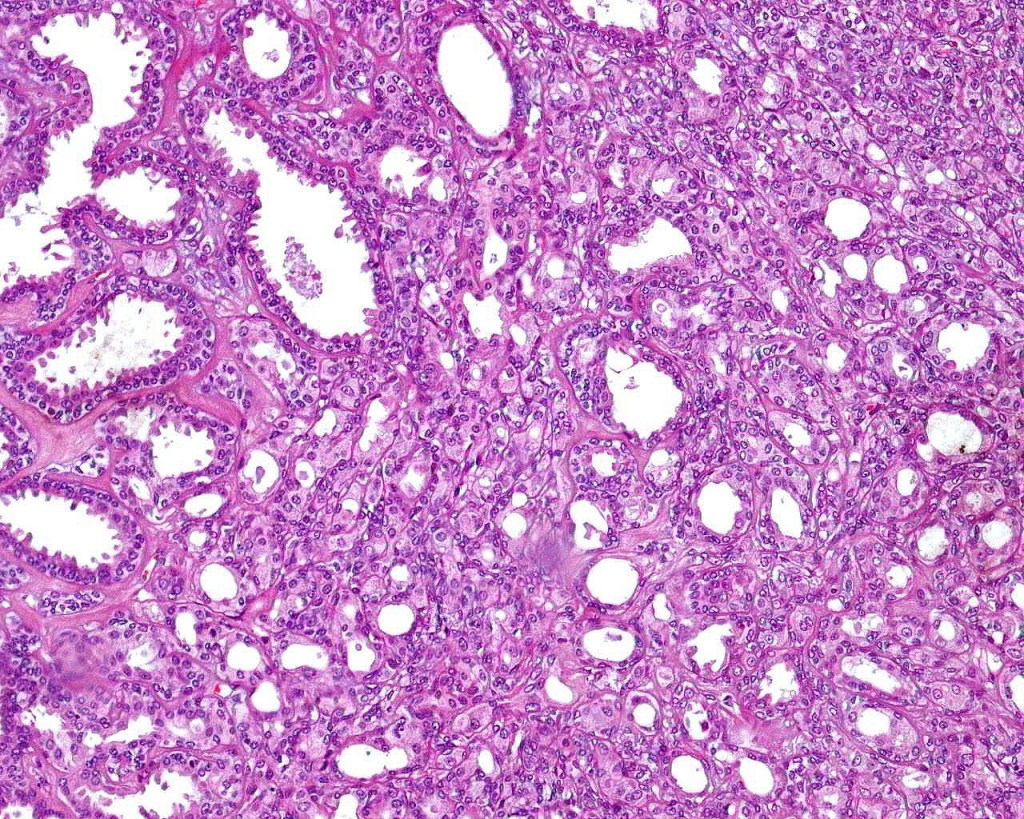
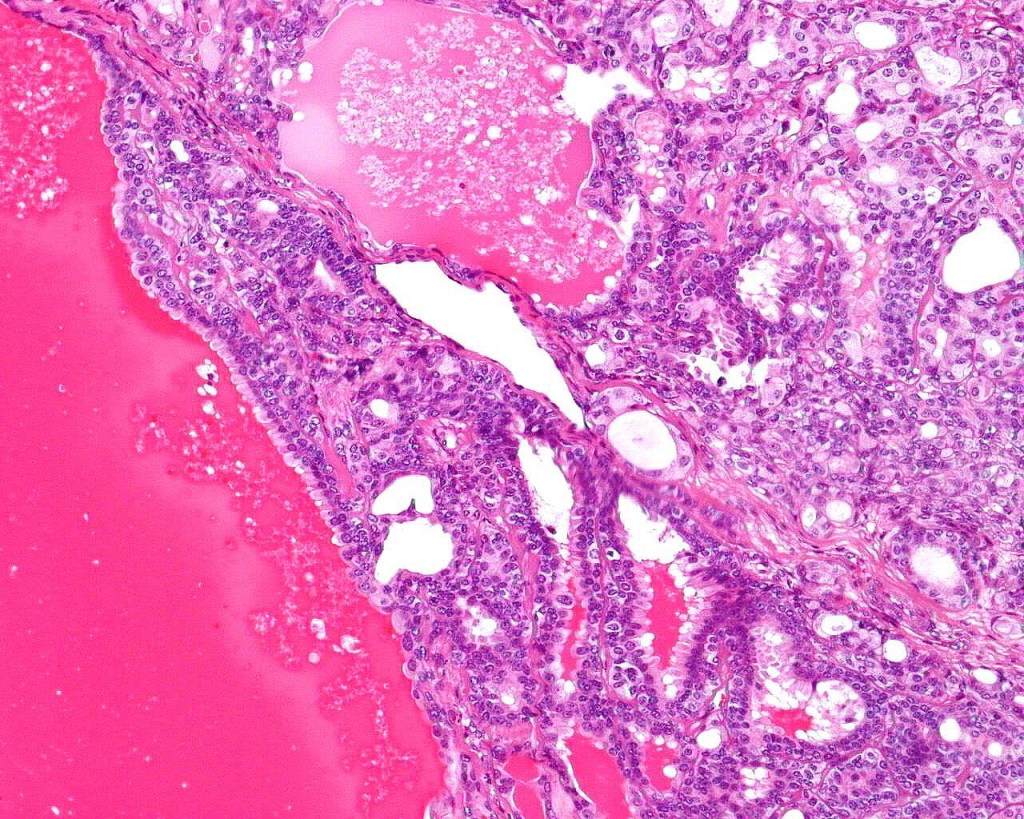
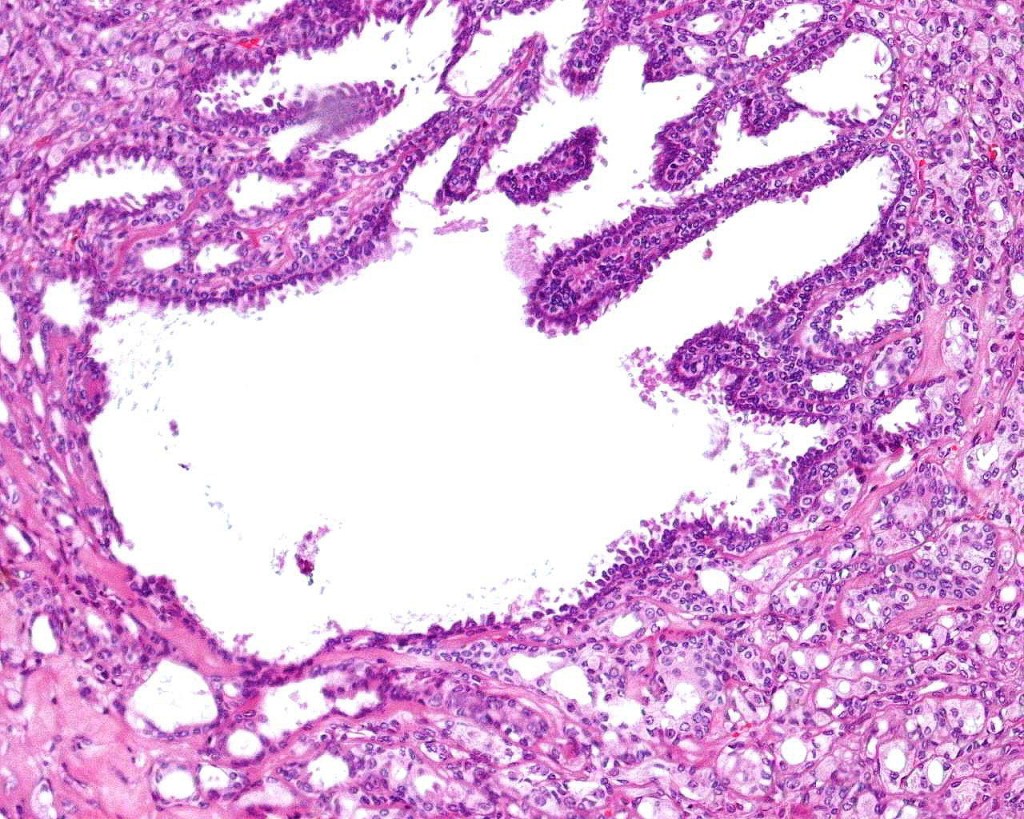
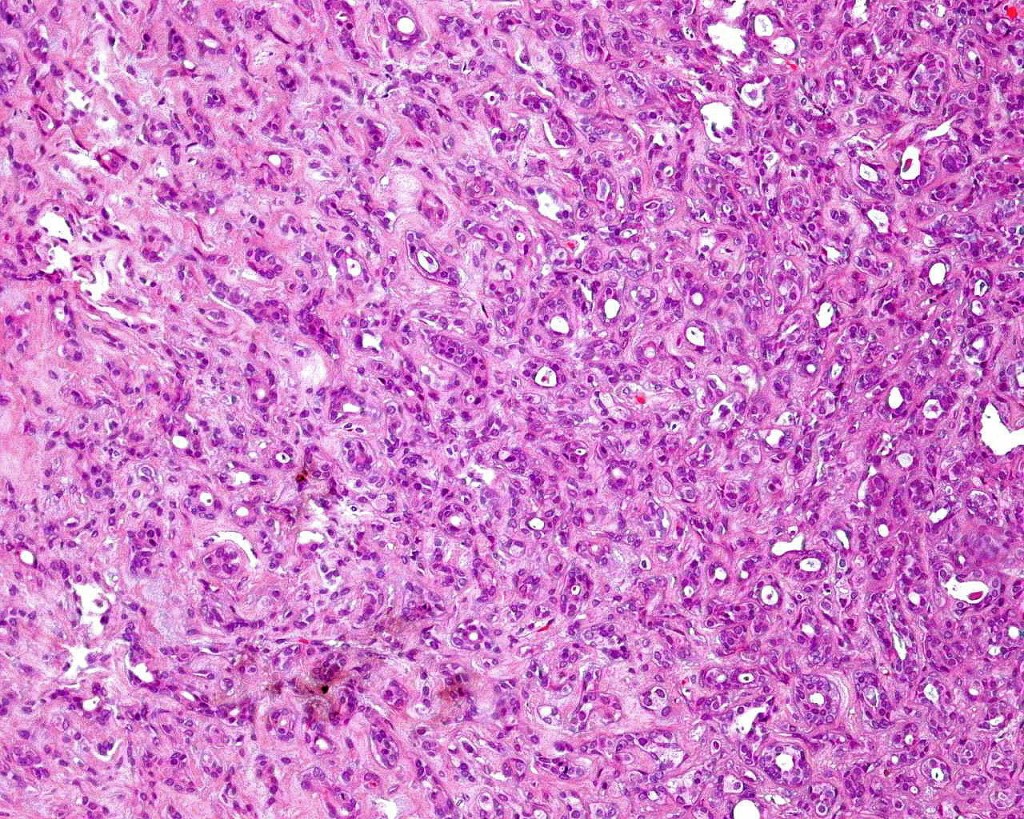
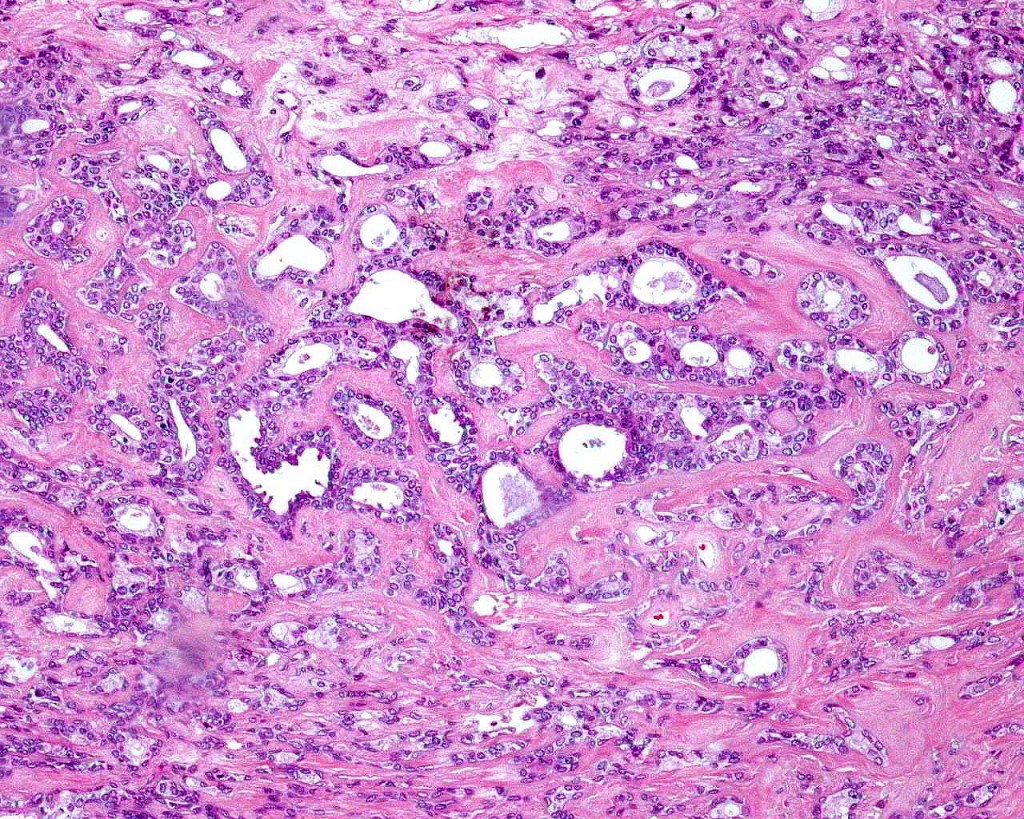
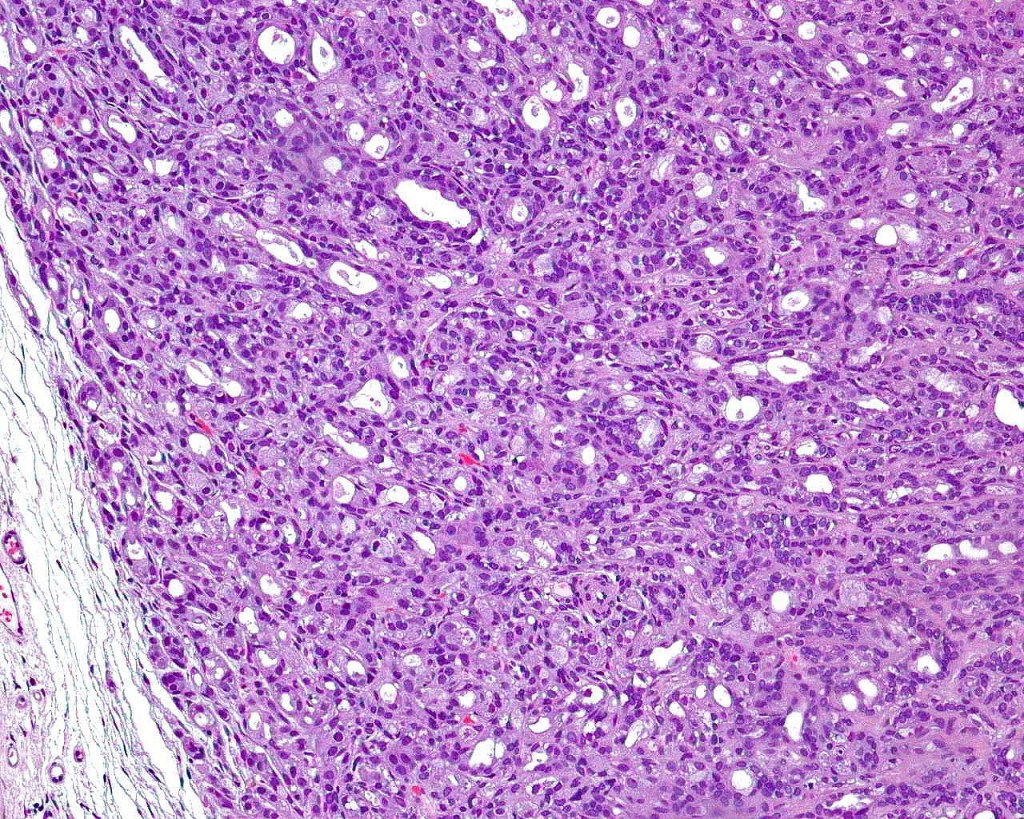
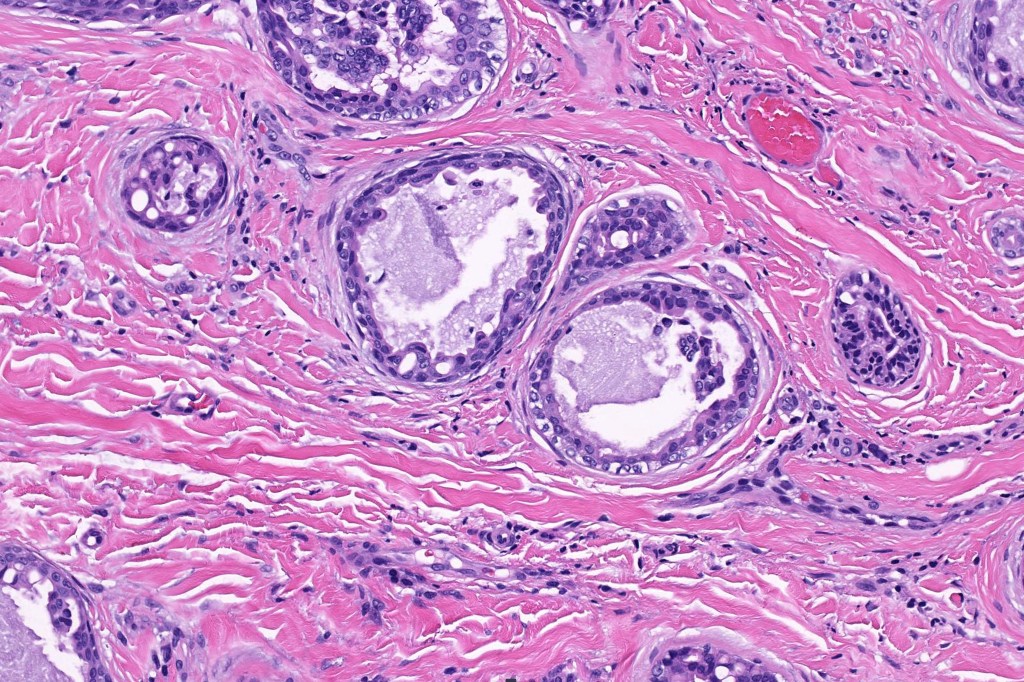
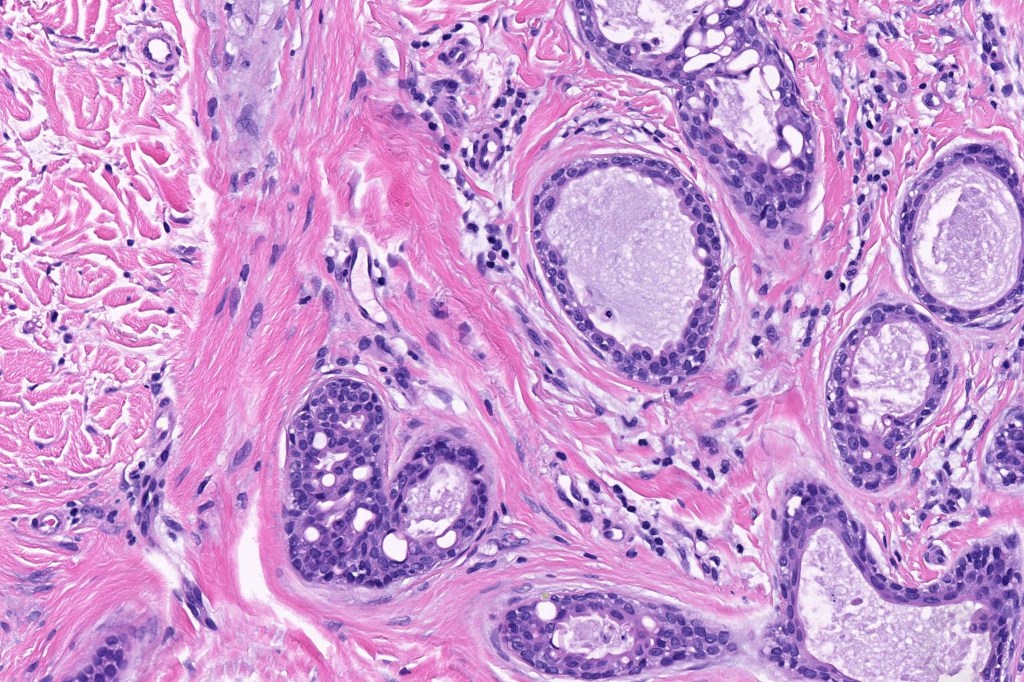
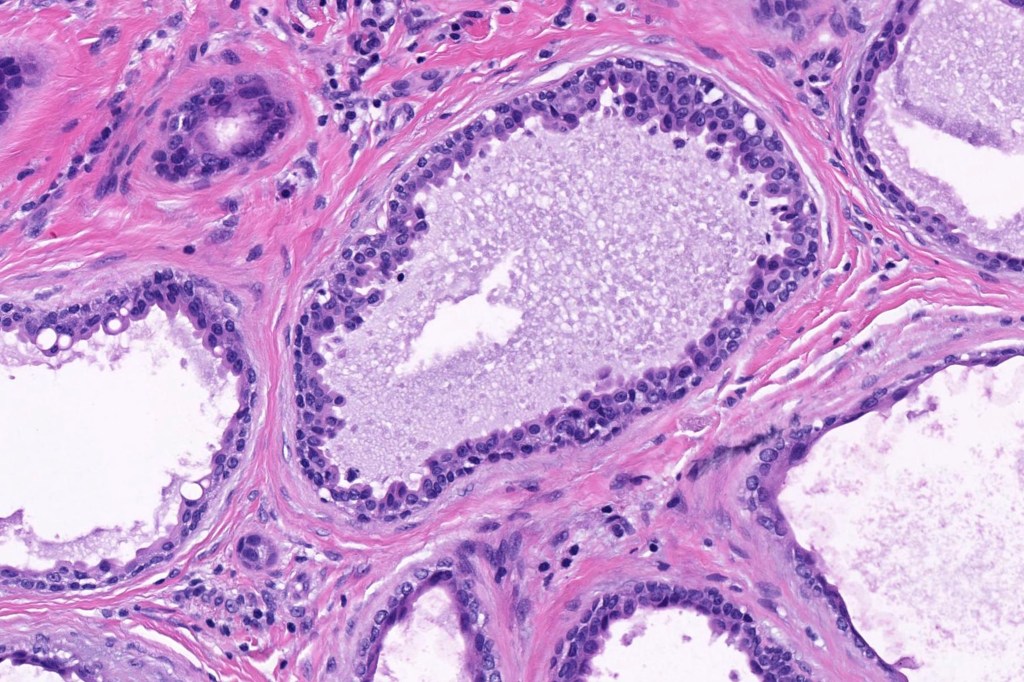
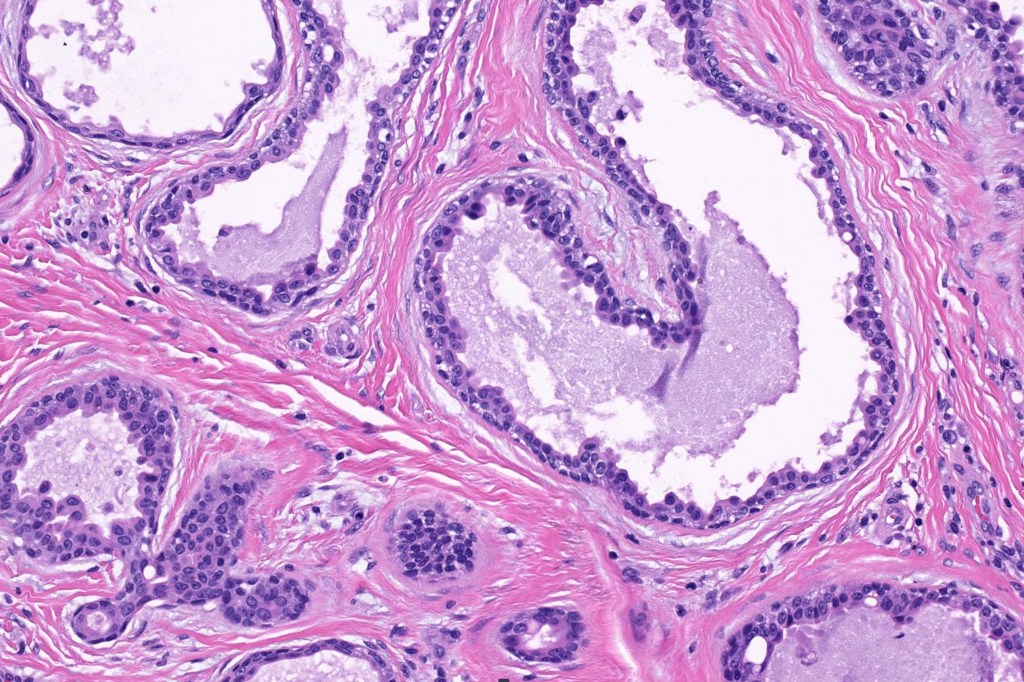
•Double-layered glands with outer myoepithelial cells and inner layer of cuboidal/columnar cells showing decapitation secretion
•Intraluminal pseudopapillae/papillae
•Stromal lymphocytic/plasma cell infiltrate
•Rarely sebaceous differentiation
•Luminal cells EMA, CEA, GCDFP-15, HMFG-1 +ve
•Myoepithelial cells S100, SMA, p63 +ve
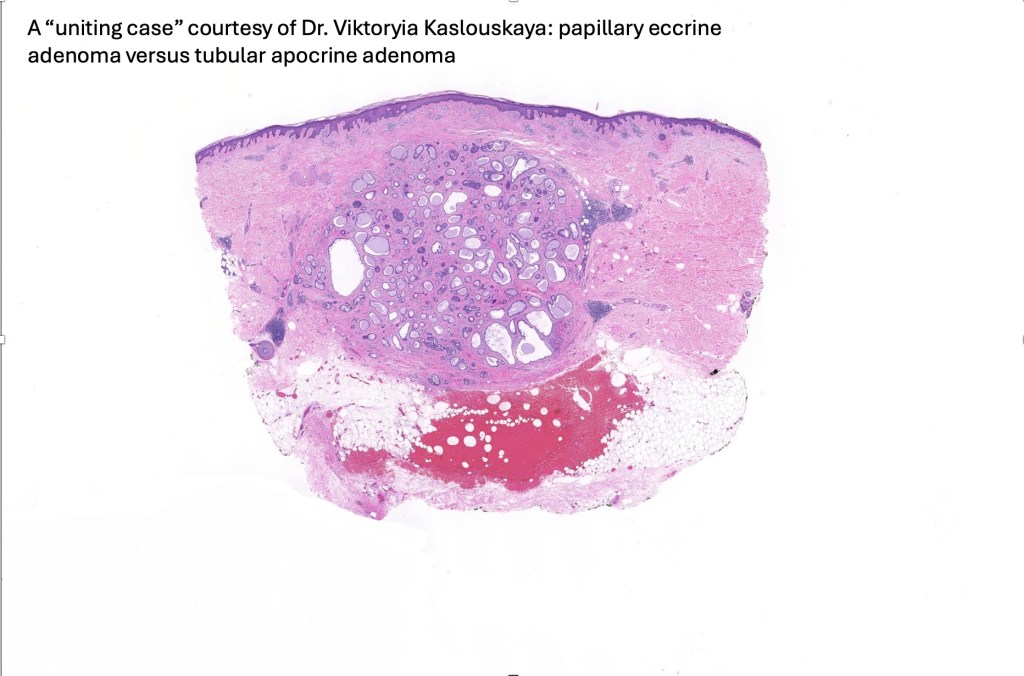
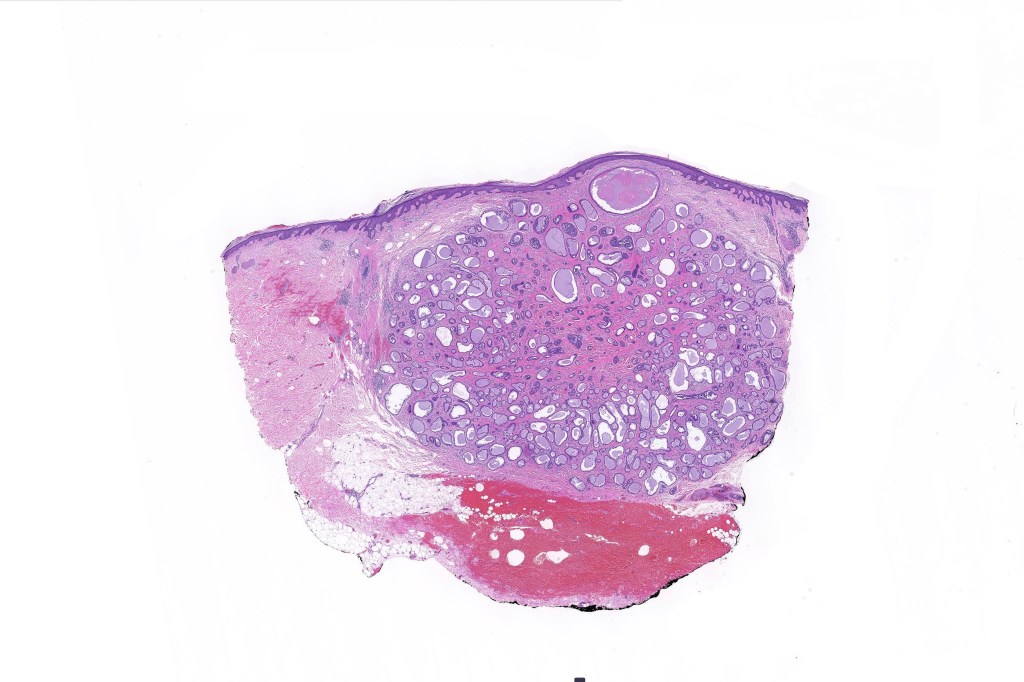
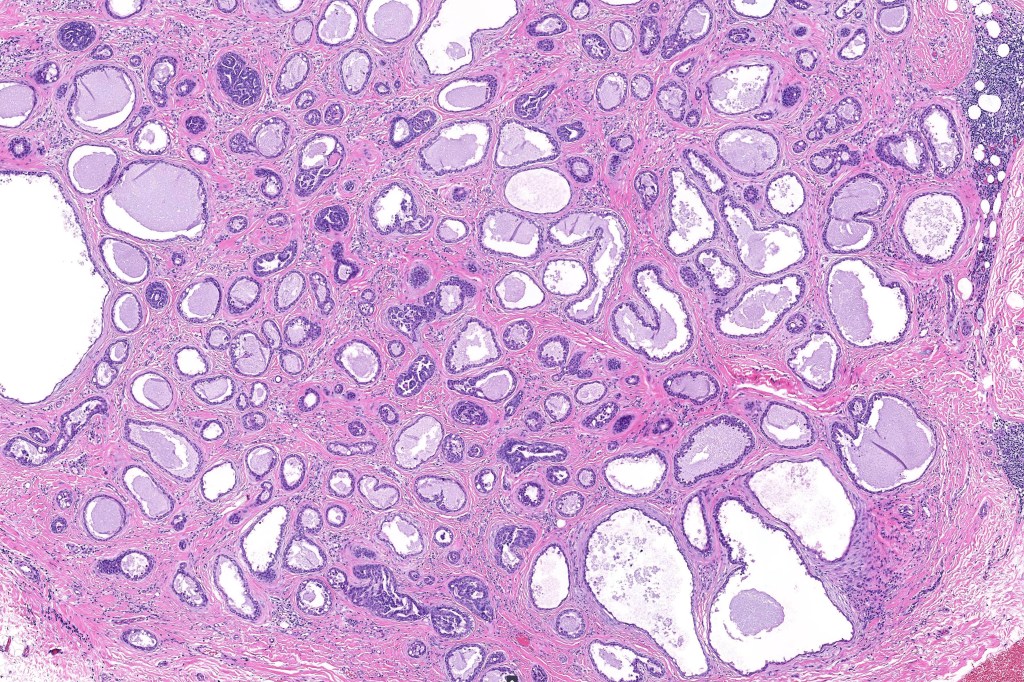
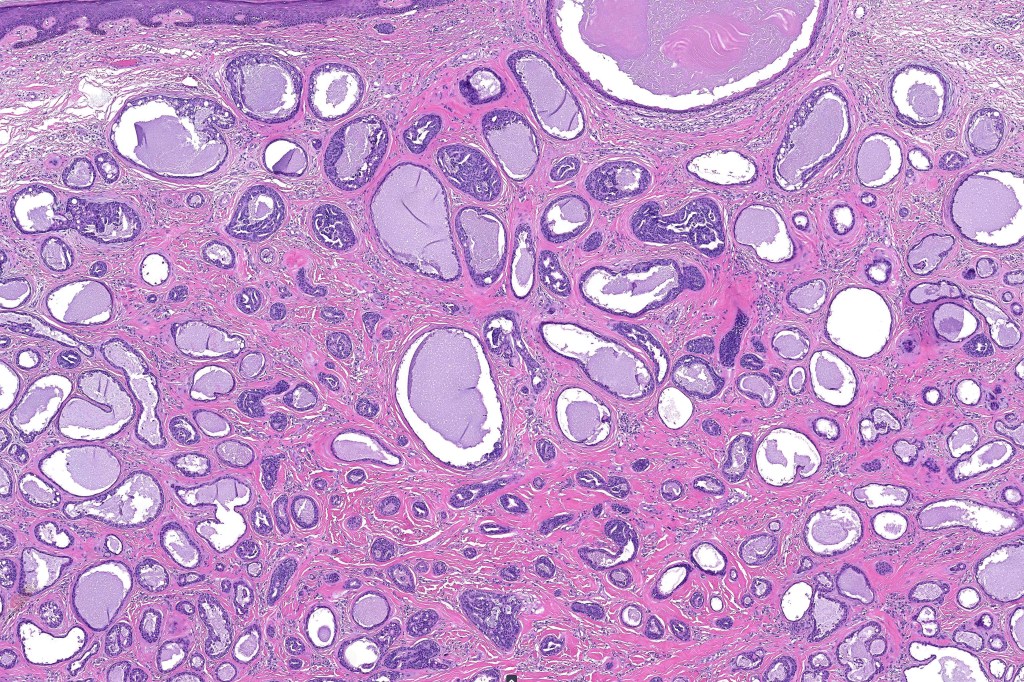
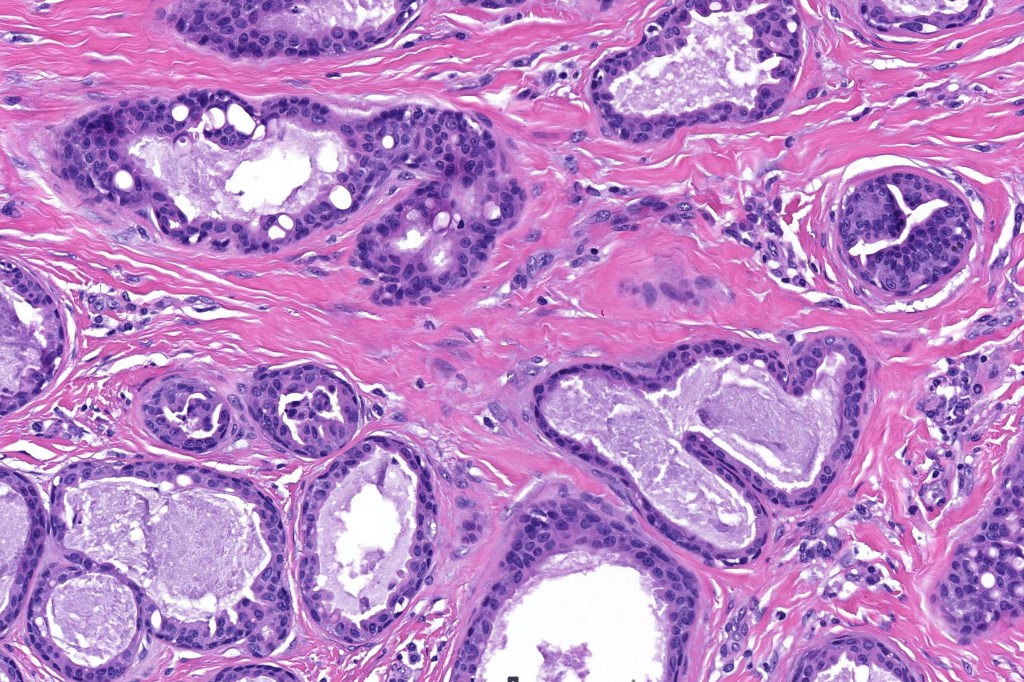
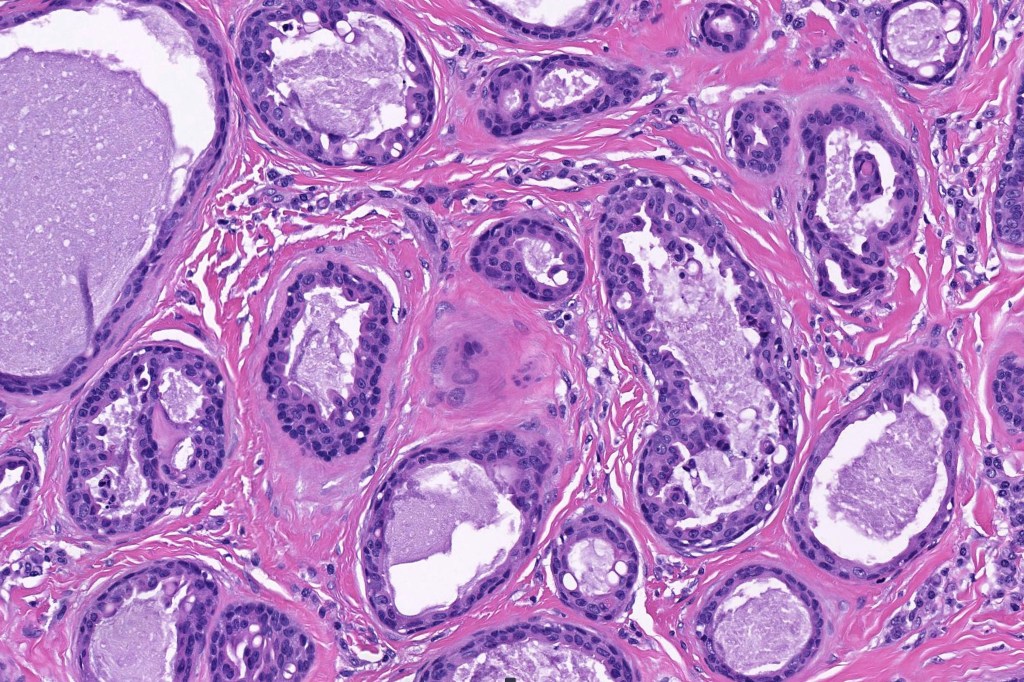
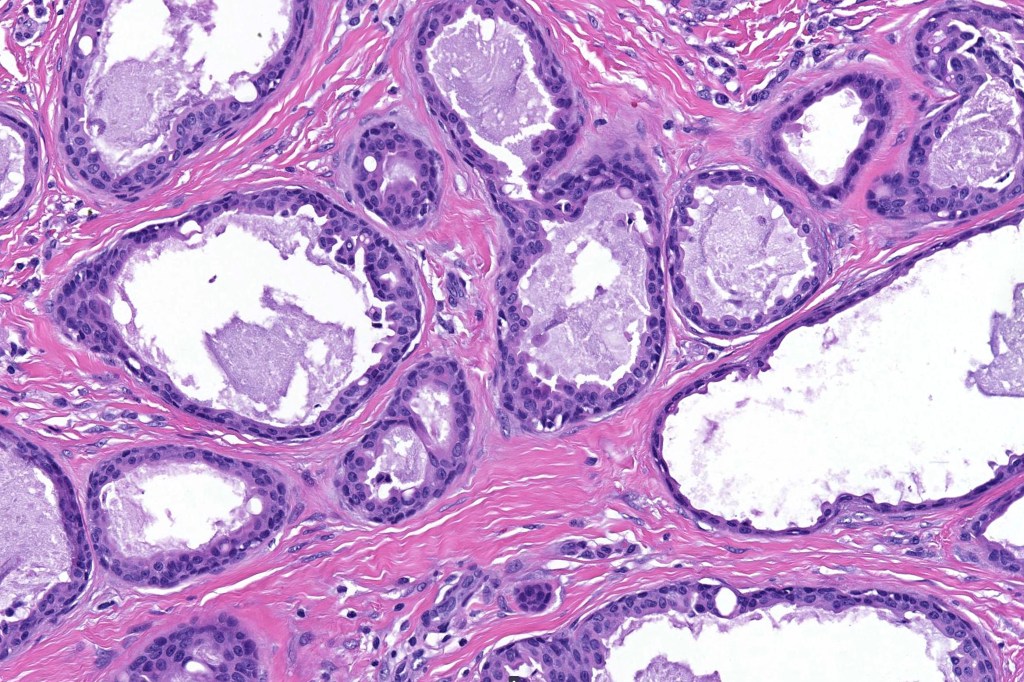
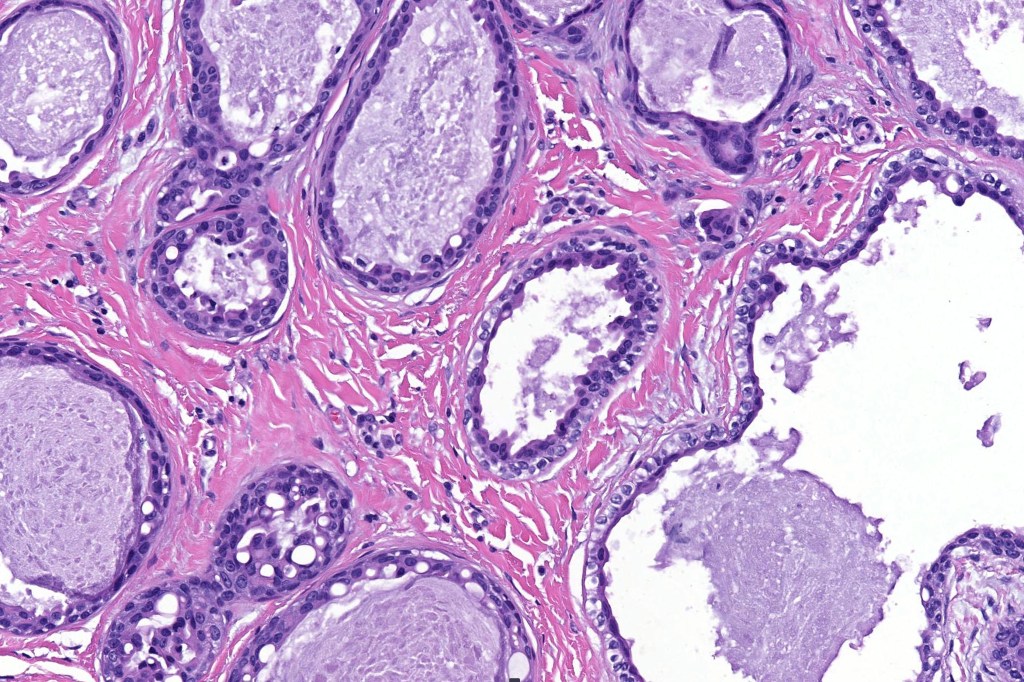
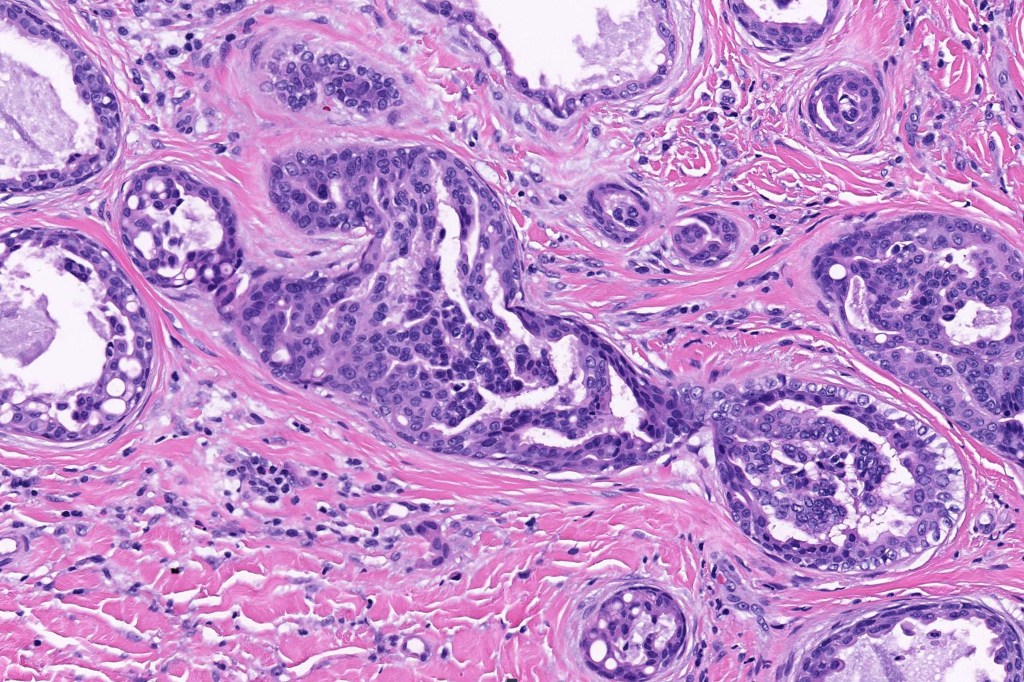
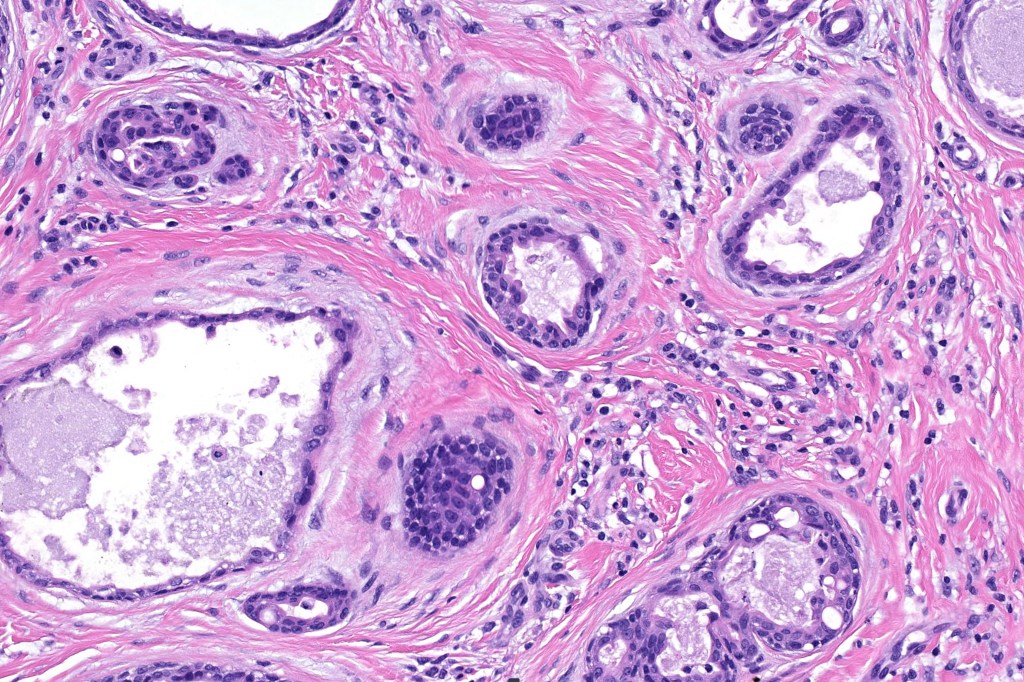
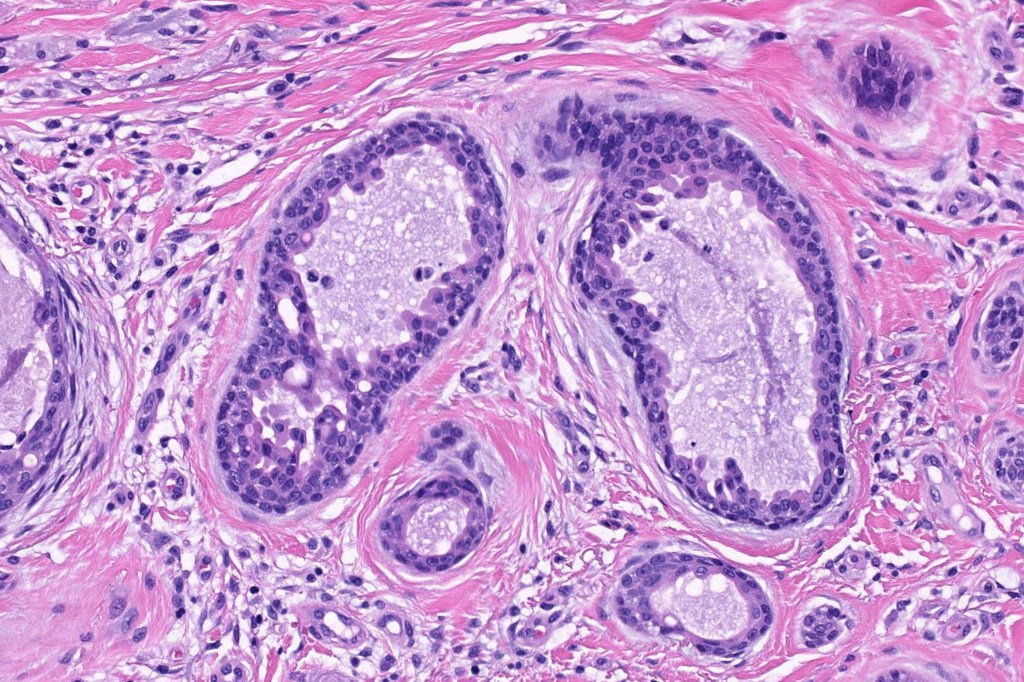
Thank you Viktoryia for sharing this fascinating case.
Leave a reply to Phillip McKee Cancel reply